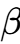The Global Evolution of GLP-1 Receptor Agonists: A Comprehensive Analysis of Mechanisms, Clinical Multipotency, and Societal Implications
The pharmacological landscape of metabolic and chronic disease is currently undergoing a paradigm shift driven by the emergence of glucagon-like peptide-1 (GLP-1) receptor agonists. Originally conceptualized in the late 20th century as specialized therapies for glycemic control in type 2 diabetes mellitus (T2DM), these agents have evolved into multi-organ stabilizers with profound implications for obesity, cardiovascular health, renal function, hepatology, and neuropsychiatric disorders.1 The clinical trajectory of GLP-1 drugs represents one of the most significant advancements in modern medicine, transitioning from a niche endocrine intervention to a "whole-body" medication class that addresses the underlying inflammatory and metabolic drivers of global morbidity.2 This report provides an exhaustive investigation into the molecular mechanisms, autonomic regulation, clinical efficacy, and the future trajectory of GLP-1 therapies within an increasingly sedentary global society.
The Molecular Architecture of GLP-1 Agonists
To understand the transformative potential of GLP-1 receptor agonists (GLP-1RAs), one must first examine the endogenous hormone they mimic. GLP-1 is a member of the incretin family, peptide hormones secreted by the enteroendocrine L-cells of the small intestine and colon in response to nutrient ingestion.1 The discovery of GLP-1 can be traced back to 1981, when it was isolated from the pancreatic islets of the anglerfish, eventually leading to its identification in the mammalian gut mucosa.1
Mechanism of Action and Glucose Homeostasis
Endogenous GLP-1 performs several vital functions to maintain metabolic equilibrium. Upon secretion, it binds to the GLP-1 receptor (GLP-1R), a seven-transmembrane G protein-coupled receptor found in high densities within the pancreas, brain, heart, and lungs.1 The activation of GLP-1R initiates a complex intracellular signaling cascade, primarily increasing the production of cyclic adenosine monophosphate (cAMP) and activating the protein kinase A (PKA) pathway.1 In the pancreatic beta cells, this process stimulates glucose-dependent insulin secretion, a mechanism that significantly reduces the risk of hypoglycemia because insulin is only released when blood glucose levels are elevated.1
Simultaneously, GLP-1 inhibits the secretion of glucagon from pancreatic alpha cells, thereby reducing hepatic glucose output.1 Beyond these hormonal effects, GLP-1 significantly impacts gastrointestinal (GI) physiology. It slows the rate of gastric emptying, which prolongs the sensation of satiety and dampens postprandial glucose excursions.5 However, the therapeutic utility of natural GLP-1 is limited by its exceptionally short half-life of 1 to 2 minutes, as it is rapidly degraded by the enzyme dipeptidyl peptidase-4 (DPP-4).1 Synthetic GLP-1RAs are engineered to resist this enzymatic degradation, allowing for prolonged therapeutic windows that range from daily to weekly administration.1
The Evolution of Incretin Targets
The field has moved beyond simple GLP-1 mimicry to multi-receptor agonism. Modern therapies now target additional incretin pathways, such as the glucose-dependent insulinotropic polypeptide (GIP) and the glucagon receptor.11 GIP is another gut-derived hormone that stimulates insulin secretion, but in the context of dual agonism (e.g., Tirzepatide), it appears to potentiate the weight-loss and appetite-suppressant effects of GLP-1 while potentially mitigating some gastrointestinal side effects.6 Triple agonists currently in clinical trials (e.g., Retatrutide) further incorporate glucagon receptor agonism, which increases energy expenditure and fat oxidation, potentially achieving "bariatric-like" weight loss outcomes.13
Autonomic Regulation: The Gut-Brain-Heart Axis
The brain system most directly and extensively affected by GLP-1 drugs is the autonomic nervous system, specifically the interface between the parasympathetic nervous system (PSNS) and the sympathetic nervous system (SNS).15 This interaction is primarily mediated through the vagus nerve and central autonomic nuclei in the brainstem.9
The Parasympathetic Nervous System (PSNS) and Vagal Control
The PSNS, often characterized as the "rest and digest" system, is the primary conduit for the early-phase release of GLP-1.9 Surgical lesioning of the subdiaphragmatic vagus nerve or the administration of muscarinic receptor antagonists (which block acetylcholine, the primary PSNS neurotransmitter) has been shown to prevent GLP-1 release in response to intestinal glucose.9 This suggests that GLP-1 secretion is not merely a local response to nutrients but is part of a "top-down" neural circuit controlled by the brain.9
Within the brainstem, GLP-1 receptors are found in the nucleus tractus solitarius (NTS) and the nucleus ambiguus.1 Research using the long-lasting agonist Exendin-4 has demonstrated that central GLP-1R stimulation actually diminishes parasympathetic modulation of the heart.15 Specifically, the drugs decrease both excitatory glutamatergic and inhibitory glycinergic neurotransmission to preganglionic parasympathetic cardiac vagal neurons.15 This reduction in PSNS tone at the sinoatrial (SA) node results in a characteristic increase in resting heart rate observed in many patients.15
Contrasting the Sympathetic vs. Parasympathetic Systems
The Sympathetic Nervous System (SNS) generally acts in opposition to the PSNS, preparing the body for "fight or flight" by increasing heart rate and suppressing digestion. The interplay between GLP-1RAs and these two systems is a critical component of their metabolic efficacy.
Feature | Parasympathetic Nervous System (PSNS) | Sympathetic Nervous System (SNS) | GLP-1RA Impact |
Primary Goal | Energy conservation, digestion, rest | Energy mobilization, stress response | Modulates both to prioritize satiety and glucose uptake.1 |
Gastric Effect | Stimulates motility and secretion | Inhibits motility and secretion | Slows gastric emptying, often through vagal modulation.7 |
Cardiac Effect | Decreases Heart Rate via M2 receptors | Increases Heart Rate via | Increases Heart Rate by diminishing PSNS cardiac tone.15 |
Vascular Effect | Minimal influence | Vasoconstriction; Increases BP | Generally reduces BP via reduced sympathoexcitation.1 |
Regulatory Conduit | Vagus Nerve (Cranial Nerve X) | Sympathetic Chain Ganglia | Vagal afferents are essential for satiety signaling.9 |
Interestingly, while GLP-1RAs increase heart rate (a typically sympathetic-like effect), they simultaneously reduce sympathetic nervous system activity at the carotid body.6 This reduction in sympathoexcitation is a primary reason why these drugs effectively lower systolic blood pressure and provide cardiovascular protection, even in patients without diabetes.1
Sleep Health: Mechanical and Metabolic Restoration
Sleep disturbances, particularly obstructive sleep apnea (OSA), are intrinsically linked to metabolic dysfunction and obesity. GLP-1RAs are currently transforming the management of OSA by addressing both the mechanical and neurological drivers of the disorder.6
Obstructive Sleep Apnea and Weight-Mediated Relief
Obesity is a major risk factor for OSA because fatty tissue deposits in the neck and tongue narrow the airway, making it susceptible to collapse during sleep.21 The weight loss achieved through GLP-1 and dual agonists (averaging 15–20%) significantly reduces these pharyngeal obstructions.8 In the SURMOUNT-OSA trial, Tirzepatide demonstrated a statistically significant reduction in the apnea-hypopnea index (AHI), which measures the number of breathing interruptions per hour.6 Patients treated with Tirzepatide saw an average reduction of 29.3 events per hour, compared to only 5 events in the placebo group.17
Beyond the reduction of fatty tissue, weight loss improves end-expiratory lung volume (EELV). Increased EELV raises "caudal traction" on the upper airway, essentially pulling the airway open from below and preventing collapse.6 This combination of reduced upper airway resistance and improved lung volume has led the FDA to approve Tirzepatide specifically for the treatment of moderate to severe OSA.10
Sleep Architecture and Circadian Regulation
Emerging research suggests that GLP-1RAs may directly influence sleep architecture—the cycle of REM and deep sleep stages—through central nervous system signaling.26 GLP-1 receptors are abundant in the hypothalamus, the brain's primary regulator of the sleep-wake cycle.17
- Deep Sleep Quality: Many patients report fewer nighttime awakenings and feeling more refreshed in the morning.24 This suggests that by stabilizing blood glucose levels, the drugs prevent nocturnal hypoglycemia and restlessness, facilitating longer periods of deep NREM sleep.26
- Circadian Rhythm Restoration: GLP-1 secretion naturally follows a circadian rhythm, which is often blunted in individuals with metabolic disease.27 By restoring these patterns, GLP-1RAs may help align the body's internal clock, making it easier to fall asleep and wake up naturally.24
- Neuroprotection: Chronic sleep apnea leads to brain injury through intermittent hypoxia and neuroinflammation. GLP-1RAs exhibit anti-inflammatory effects in the brain (potentially via the Nrf2/HO-1 and MAPK/NF-κB pathways), which may protect neural tissue from the oxidative stress caused by OSA.6
Modulating Reward: Addictive Impulses and Cravings
One of the most profound observations in GLP-1 research is the drugs' ability to reduce "food noise"—the constant, intrusive preoccupation with eating.8 This effect stems from GLP-1R activation in the brain's reward centers, particularly the ventral tegmental area (VTA) and the nucleus accumbens (NAc).28
The Dopamine Theory of GLP-1 Intervention
Addictive substances and high-calorie foods "hijack" the mesolimbic dopamine pathway, producing dopamine levels far greater than natural stimuli.31 This leads to compulsive behaviors and impaired decision-making.31 GLP-1 receptors are expressed in these reward-related regions, where their activation blunts the release of dopamine in response to addictive substances.28
Substance | Preclinical/Clinical Findings | Mechanism of Effect |
Alcohol | Reduced intake, motivation, and relapse in rats; reduced heavy drinking days in humans with BMI > 30.28 | Blocks alcohol-induced dopamine increase in the NAc; acts on the LDTg.28 |
Nicotine | Attenuated self-administration and withdrawal-induced hyperphagia in rodents.28 | Enhances excitatory drive in the medial habenula, promoting drug avoidance.29 |
Opioids | Decreased craving in small clinical trials; exendin-4 reduced drug-seeking in rats.28 | Modulates mesolimbic dopaminergic signaling; potentially activates inhibitory GABA neurons in the VTA.28 |
Stimulants | Reduced responding for cocaine and amphetamines in rodent models.28 | Damps reward signaling and reduces conditioned responses.28 |
Crucially, DPP-4 inhibitors (which increase endogenous GLP-1 levels) do not appear to have this effect on addiction, suggesting that the supraphysiological doses provided by GLP-1 agonists are necessary to access the specific central reward circuits involved in substance use disorders.28
Pleiotropic Benefits: Beyond Glycemic Control
The broad distribution of GLP-1 receptors across multiple organ systems accounts for the drugs' wide-ranging "secondary" benefits, many of which are partly independent of weight loss.1
Cardiovascular Protection and Heart Failure
Large-scale Cardiovascular Outcome Trials (CVOTs) have established that GLP-1RAs significantly reduce the risk of major adverse cardiovascular events (MACE), including cardiovascular death, non-fatal myocardial infarction, and non-fatal stroke.1
- The SELECT Trial: Conducted in adults with obesity and established cardiovascular disease but without diabetes, this trial showed a 20% reduction in MACE events over 40 months.2
- Heart Failure (HFpEF): In patients with heart failure with preserved ejection fraction (HFpEF), semaglutide and tirzepatide have demonstrated significant improvements in physical limitations, exercise function (as measured by the 6-minute walk test), and quality of life scores.2
Renal and Hepatic Health
The kidneys and liver are major beneficiaries of GLP-1RA therapy. The FLOW trial demonstrated that semaglutide reduces the risk of kidney disease progression and death from kidney-related causes by 24% in adults with T2D and CKD.2 In the liver, GLP-1RAs address metabolic dysfunction-associated steatohepatitis (MASH). In the ESSENCE trial, semaglutide 2.4 mg led to the resolution of steatohepatitis in 62.9% of patients, compared to 34.3% with placebo.2 While hepatocytes do not express GLP-1 receptors, the benefits are likely mediated through reduced systemic inflammation and improved lipid metabolism.2
Peripheral Artery Disease and Osteoarthritis
Recent trials have expanded the indications to physical mobility. The STRIDE trial found that semaglutide significantly increased the maximum walking distance in patients with peripheral artery disease (PAD).2 Similarly, the STEP 9 trial showed that semaglutide improved WOMAC pain scores by 41.7 points in patients with knee osteoarthritis and obesity.2
Comparative Analysis: Drugs on the Market vs. The Pipeline
The current therapeutic landscape is categorized by increasing potency and multi-receptor targeting.14
Drug Name | Class | Formulation | Primary Indication | Weight Loss Potency |
Liraglutide (Saxenda) | GLP-1 Agonist | Daily SC | Obesity/T2D | 5% – 10% 8 |
Semaglutide (Wegovy) | GLP-1 Agonist | Weekly SC | Obesity/T2D/CV Risk | 15% – 20% 23 |
Semaglutide (Rybelsus) | GLP-1 Agonist | Daily Oral | T2D (Weight loss pending) | Moderate 10 |
Tirzepatide (Zepbound) | Dual GLP-1/GIP | Weekly SC | Obesity/T2D/OSA | 20% – 22.5% 11 |
Retatrutide (In Trials) | Triple Agonist | Weekly SC | Obesity/T2D | 24% – 25% 11 |
Emerging Drug Candidates
The pharmaceutical pipeline is heavily invested in non-invasive delivery and enhanced metabolic impact.
- Orforglipron (Eli Lilly): An oral, small-molecule GLP-1RA currently in Phase 3 trials. Unlike oral semaglutide, it does not require strict fasting and could significantly broaden market access.4
- Maritide (Amgen): A dual GIPR antagonist and GLP-1R agonist that may offer more durable weight loss with less frequent dosing.10
- Survodutide (Boehringer Ingelheim): A dual GLP-1 and glucagon receptor agonist showing significant promise in treating MASH.2
Risks, Adverse Events, and Strategic Vigilance
While the benefits are extensive, GLP-1RAs carry specific risks that necessitate careful clinical monitoring.22
Gastrointestinal and Systemic Effects
The most common adverse events are gastrointestinal, including nausea, vomiting, diarrhea, bloating, and constipation.22 While usually mild to moderate and occurring during dose titration, they can occasionally lead to more severe complications like pancreatitis or bowel obstruction.22 Data from the FAERS database suggests that Tirzepatide may have a significantly higher risk of hospitalizations (RR 3.13) compared to older agents like Liraglutide, though it shows a lower risk of hepatobiliary and certain infections.35
Muscle and Bone Integrity
A critical concern in GLP-1-mediated weight loss is the preservation of lean muscle mass. Studies indicate that rapid weight reduction can lead to a 15–25% loss of lean muscle mass, which can lower metabolic rates and physical strength.8 Future R&D is increasingly focusing on "quality weight loss" by combining GLP-1RAs with myostatin inhibitors (ActRII pathway) to protect muscle while deepening fat loss.14
The Societal Paradigm: Sedentary Lifestyles and Future Solutions
As societies become increasingly sedentary and calorie-dense, GLP-1 medications are transitioning from medical treatments to "social technologies" that reshape bodies and identities.37
The Possibility of Lifelong Medication Trends
The emergence of "medicated societies" is becoming a viable outcome of current lifestyle trends. ASU researchers have identified nine global trends emerging from massive GLP-1 use, including a profound sense of "normality" described by users after weight loss, and a willingness to endure side effects and financial sacrifices to maintain access.37 This has led to "medication tinkering" and unregulated use through telehealth platforms, often driven by aesthetic "weight anxiety" rather than clinical necessity.37 The medicalization of weight may ironically intensify weight stigma, as those who do not use the drugs may be judged more harshly in a culture that views weight as an easily "fixable" problem.38
Alternative Technologies to Reduce Dependence
To prevent widespread dependence on pharmaceutical interventions, several alternative technologies and care models are emerging:
- Digital Therapeutics and AI: Platforms that provide personalized behavioral support and "precision nutrition" can help patients maintain weight loss achieved through drugs or lifestyle alone.8
- Home-Based Sleep and Metabolic Monitoring: Tools like Wesper’s home sleep diagnostics allow for earlier identification of metabolic and sleep disorders, enabling targeted treatment plans that might not require medication if caught early.20
- Advanced Exercise Technology: Physician-referred supervised exercise programs that utilize advanced equipment can assist with chronic disease management, potentially offering a mechanical and biological alternative to GLP-1 agonism for metabolic syndrome.39
- Food System Innovation: The rise of GLP-1RAs is creating opportunities for food companies to finally build healthier food systems that prioritize satiety and nutrient density over hyper-palatability.8
Conclusion
GLP-1 receptor agonists have fundamentally reordered the management of chronic, metabolic, and inflammatory diseases. By leveraging the body's own incretin system and modulating the delicate balance of the autonomic nervous system, these drugs offer a multipotent solution to modern healthcare challenges—from cardiovascular and renal decline to sleep apnea and addiction.2 However, the transition toward a "medicated society" demands scientific and ethical vigilance. The future of GLP-1 research lies in refining multi-agonist molecules, ensuring the preservation of lean muscle mass, and integrating these pharmaceutical breakthroughs with digital and lifestyle technologies to ensure that weight loss translates into lasting, sustainable health.8
Works cited
- The benefits of GLP1 receptors in cardiovascular diseases - PMC - NIH, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10739421/
- The expanding benefits of GLP-1 medicines - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12281309/
- Current Perspectives on GLP-1 Agonists in Contemporary Clinical Practice from Science and Mechanistic Foundations To Optimal Translation - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12511252/
- Outlook for Obesity in 2026: From Consolidation to Acceleration ..., accessed February 18, 2026, https://www.iqvia.com/locations/emea/blogs/2026/01/outlook-for-obesity-in-2026
- Are GLP-1 Drugs the Future of Alcohol Addiction Treatment? - News-Medical, accessed February 18, 2026, https://www.news-medical.net/health/Are-GLP-1-Drugs-the-Future-of-Alcohol-Addiction-Treatment.aspx
- Glucagon-like peptide-1 receptor agonists for the treatment of ..., accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12538296/
- Effects of glucagon-like peptide-1 and sympathetic stimulation on gastric accommodation in humans - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC2538797/
- UC Davis Health examines systemic impact of GLP-1–based therapies, accessed February 18, 2026, https://health.ucdavis.edu/news/headlines/uc-davis-health-examines-systemic-impact-of-glp-1based-therapies/2025/12
- Reappraising the role of the vagus nerve in GLP‐1‐mediated ..., accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC8714868/
- GLP-1 Pipeline Update: November 2025 - Prime Therapeutics - Portal, accessed February 18, 2026, https://www.primetherapeutics.com/glp-1-pipeline-update-november-2025
- How does retatrutide compare to tirzepatide? - Drugs.com, accessed February 18, 2026, https://www.drugs.com/medical-answers/how-retatrutide-compare-tirzepatide-3580916/
- Retatrutide vs. Tirzepatide: Weight Loss Medication Compared | Mochi Health, accessed February 18, 2026, https://joinmochi.com/blogs/retatrutide-vs-tirzepatide
- SUN-659 Comparative Efficacy and Safety of Tirzepatide vs Retatrutide in Weight Loss: A Network Meta-Analysis of Clinical Trials - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12544991/
- Patent and Innovation Trends in GLP-1 and Weight Loss Drugs (2020–2025): What the IP and Science Signal Next | Cypris, accessed February 18, 2026, https://www.cypris.ai/insights/patent-and-innovation-trends-in-glp-1-and-weight-loss-drugs-2020-2025-what-the-ip-and-science-signal-next
- GLP-1 receptor stimulation depresses heart rate variability and inhibits neurotransmission to cardiac vagal neurons - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC3002870/
- GLP-1 receptor stimulation depresses heart rate variability and inhibits neurotransmission to cardiac vagal neurons - PubMed, accessed February 18, 2026, https://pubmed.ncbi.nlm.nih.gov/20736238/
- (PDF) The Application of GLP-1 Receptor Agonists and SGLT2 ..., accessed February 18, 2026, https://www.researchgate.net/publication/387687614_The_Application_of_GLP-1_Receptor_Agonists_and_SGLT2_Inhibitors_in_Obstructive_Sleep_Apnea_Breakthrough_or_Overhyped
- Reappraising the role of the vagus nerve in GLP-1-mediated regulation of eating - PubMed, accessed February 18, 2026, https://pubmed.ncbi.nlm.nih.gov/34185884/
- Thieme Test Prep for the USMLE®: Medical Physiology Q&A [1st ed.] 1626233845, 9781626233843, 9781626233850 - DOKUMEN.PUB, accessed February 18, 2026, https://dokumen.pub/thieme-test-prep-for-the-usmle-medical-physiology-qampa-1stnbsped-1626233845-9781626233843-9781626233850.html
- Transforming Sleep & Metabolic Health with GLP-1 Medications - Wesper, accessed February 18, 2026, https://wesper.co/blogs/wesper-journal/transforming-sleep-and-metabolic-health-with-glp-1-medications
- GLP-1 Drugs Might Help Quell Sleep Apnea - Powers Health, accessed February 18, 2026, https://www.powershealth.org/about-us/newsroom/health-library/2026/01/05/glp-1-drugs-might-help-quell-sleep-apnea
- GLP-1s for Sleep Apnea - Sleep Foundation, accessed February 18, 2026, https://www.sleepfoundation.org/sleep-apnea/glp-1-for-sleep-apnea/
- Study Details | NCT07281196 | Semaglutide Effects on Sleep Apnea in Patients With Type 2 Diabetes/Obesity and Comorbid Obstructive Sleep Apnea | ClinicalTrials.gov, accessed February 18, 2026, https://clinicaltrials.gov/study/NCT07281196
- Can GLP-1 Improve Sleep Quality? Research & Benefits - Yorktown Health Vernon Hills, accessed February 18, 2026, https://yorktownhealthvh.com/blog/can-glp-1-improve-sleep-quality/
- The impact of GLP-1 agonists on sleep disorders: spotlight on sleep apnea - PubMed, accessed February 18, 2026, https://pubmed.ncbi.nlm.nih.gov/41114602/
- The Hidden Link Between Semaglutide, Tirzepatide, Immune System, and Better Sleep - Austin MD Aesthetics & Wellness, accessed February 18, 2026, https://austinmdclinic.com/link-between-semaglutide-tirzepatide-immune-system-and-sleep/
- Sleep is increased by Liraglutide, a Glucagon-Like Peptide-1 Receptor Agonist, in rats | Request PDF - ResearchGate, accessed February 18, 2026, https://www.researchgate.net/publication/365630621_Sleep_is_increased_by_Liraglutide_a_Glucagon-Like_Peptide-1_Receptor_Agonist_in_rats
- Substance Use Disorder and Alcohol Use Disorder - Examining ..., accessed February 18, 2026, https://www.ncbi.nlm.nih.gov/books/NBK615018/
- The potential role of GLP-1 receptor agonists in substance use disorders - PMC - NIH, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12808432/
- A turning point in addiction psychiatry? | School of Public Health | Brown University, accessed February 18, 2026, https://sph.brown.edu/news/2025-07-24/brain-science-glp-1s-addiction
- 'Beyond Weight Loss': Emerging Studies Show How GLP-1 Receptor Agonists May Impact Addiction Behaviors | Pharmacy Times, accessed February 18, 2026, https://www.pharmacytimes.com/view/-beyond-weight-loss-emerging-studies-show-how-glp-1-receptor-agonists-may-impact-addiction-behaviorst
- The Real-World Clinical Benefits of GLP-1 Receptor Agonist Treatment | medRxiv, accessed February 18, 2026, https://www.medrxiv.org/content/10.1101/2025.10.24.25338256v2.full-text
- (PDF) The expanding benefits of GLP-1 medicines - ResearchGate, accessed February 18, 2026, https://www.researchgate.net/publication/393727697_The_expanding_benefits_of_GLP-1_medicines
- What's next for GLP-1 innovation: A primer on the race reshaping pharma and chronic disease care, accessed February 18, 2026, https://www.unionhealthcareinsight.com/post/glp-1-innovation-the-race-reshaping-pharma-and-chronic-disease-care
- Comparison of Safety Profile of Semaglutide, Tirzepatide, and Liraglutide in Obese Patients: FAERS Database Investigation - PMC, accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12399039/
- Pacific RxTracts - February 2026 - Scholarly Commons, accessed February 18, 2026, https://scholarlycommons.pacific.edu/cgi/viewcontent.cgi?article=1012&context=rx-tracts
- Beyond weight loss: Examining the social effects of GLP-1 medications | ASU News, accessed February 18, 2026, https://news.asu.edu/20260102-health-and-medicine-beyond-weight-loss-examining-social-effects-glp1-medications
- Beyond the prescription: Global observations on the social ..., accessed February 18, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12742762/
- 2021 FACTS AND FIGURES UNIVERSITY OF COLORADO SCHOOL OF MEDICINE, accessed February 18, 2026, https://medschool.cuanschutz.edu/docs/librariesprovider31/deans-office/facts-figures/facts-figures-2021.pdf?sfvrsn=e4f5aeba_2
- University of Colorado School of Medicine Facts and Figures CELEBRATING 137 YEARS: 1883-2020, accessed February 18, 2026, https://medschool.cuanschutz.edu/docs/librariesprovider31/deans-office/facts-figures/2020-facts-figures-annual-report.pdf?sfvrsn=2d9b83b9_2
Addendum
Pathophysiological Mechanisms and Clinical Management of Weight Loss Plateaus in GLP-1 Receptor Agonist Therapy: A Comprehensive Analysis of Metabolic Adaptation and Advanced Dosing Strategies
The pharmacological landscape of obesity management has undergone a profound transformation with the development and clinical integration of glucagon-like peptide-1 receptor agonists (GLP-1 RAs). These agents, including semaglutide and the dual GLP-1/GIP agonist tirzepatide, have demonstrated the capacity to induce weight loss previously achievable only through bariatric surgery.1 Despite these advancements, a nearly universal clinical observation is the weight loss plateau—a point at which, despite continued medication adherence and lifestyle modification, the patient’s body weight remains stationary.1 This phenomenon is not an indicator of medication failure but rather a manifestation of a sophisticated biological defense mechanism designed to maintain energy homeostasis.1 The cessation of weight loss is the result of a multifaceted interplay between metabolic adaptation, hormonal counter-regulation, and pharmacological receptor dynamics.1
The Biological Foundations of the Weight Loss Plateau
The cessation of weight loss during GLP-1 RA therapy typically manifests between six and twelve months after the initiation of treatment, frequently coinciding with the attainment of 70% to 80% of the total expected weight reduction.4 To address this stagnation, clinicians must recognize that the human body functions as a homeostatic system that perceives significant weight loss as a threat to survival.2
Metabolic Adaptation and Adaptive Thermogenesis
At the core of the weight loss plateau is metabolic adaptation, a natural biological response where the body defends its energy stores by reducing its energy expenditure.1 As a patient loses weight, their basal metabolic rate (BMR)—the energy required to maintain basic physiological functions at rest—naturally decreases because a smaller body mass requires less energy to sustain itself.7 However, the decline in energy expenditure often exceeds what would be predicted based solely on the reduction in body mass, a process termed adaptive thermogenesis.2
When caloric intake is restricted, the body increases its metabolic efficiency to conserve energy.2 This response is mediated by the hypothalamus, which integrates peripheral signals to adjust the BMR.8 Research indicates that during active weight loss, the BMR can decrease by 10% to 25%, effectively narrowing or closing the caloric deficit that was initially responsible for weight loss.4 This reduction in “calories out” eventually matches the “calories in” facilitated by the medication’s appetite suppression, leading to a state of energy equilibrium where weight loss stalls.1
Component of Energy Expenditure | Response to Weight Loss | Impact on Plateau |
Basal Metabolic Rate (BMR) | Significant Decrease | Reductions of 10-25% lower the daily caloric “burn,” necessitating further intake reductions to maintain loss.4 |
Thermic Effect of Food (TEF) | Decrease | Smaller meals result in less energy expended during digestion and nutrient processing.8 |
Non-Exercise Activity (NEAT) | Decrease | Subtle, often subconscious reductions in spontaneous movement (fidgeting, standing) to conserve energy.6 |
Exercise Energy Expenditure | Variable Decrease | Increased mechanical efficiency of movement and lower body mass reduce the caloric cost of physical activity.13 |
Hormonal Counter-Regulation and the Return of Hunger
The biological defense against weight loss is further supported by profound changes in the circulating levels of appetite-regulating hormones.2 Weight loss triggers a compensatory surge in ghrelin, the primary hunger-stimulating hormone produced in the stomach.1 Simultaneously, there is a reduction in satiety-promoting hormones such as leptin, peptide YY (PYY), and cholecystokinin (CCK).2
Leptin, produced by adipose tissue, serves as a signal to the brain regarding the state of energy stores; as fat mass decreases, leptin levels drop, signaling the hypothalamus to increase hunger and reduce energy expenditure.2 This hormonal shift creates a “tug-of-war” between the pharmacological effects of the GLP-1 RA and the body’s endogenous signals.8 Many patients report the return of “food noise”—intrusive thoughts about eating—during this period, even while maintaining their medication dose.1
Receptor Desensitization and Gastric Emptying Rebound
Pharmacological tolerance also plays a role in the emergence of plateaus. The GLP-1 receptor itself may become less responsive to a constant level of agonist stimulation over time, a process known as receptor desensitization or downregulation.1 This is a common feature of receptor-based therapies where chronic exposure to a ligand leads to a reduction in receptor density or signaling efficiency.4
Additionally, the gastrointestinal effects of GLP-1 RAs often undergo adaptation. One of the primary mechanisms for early weight loss is delayed gastric emptying, which induces a prolonged sense of fullness.1 Over several months of treatment, the stomach’s emptying rate may gradually return toward its baseline, a phenomenon called gastric emptying rebound.1 While the central effects of the medication on the brain’s appetite centers may persist, the loss of this mechanical satiety component contributes significantly to the slowing of weight loss.1
Clinical Strategies to Overcome Weight Loss Plateaus
When a weight loss plateau is reached, clinicians must evaluate several physiological and pharmacological factors to determine the most appropriate intervention. Plateaus are often a signal that the body has reached a new “set point,” and breaking through this resistance requires a multi-pronged approach.6
Pharmacological Escalation and Switching Protocols
The most direct clinical response to a weight loss stall is the titration of the medication to its maximum therapeutic dose.1 Many patients experience plateaus because they are on a sub-therapeutic dose or have not yet completed the full titration schedule, which is designed to minimize gastrointestinal side effects.3 Clinical trials, such as the STEP and SURMOUNT programs, have consistently demonstrated that higher doses of semaglutide and tirzepatide result in greater total body weight reduction.3
Medication | Starting Dose | Standard Titration Interval | Target Maintenance Dose |
Semaglutide (Wegovy) | 0.25 mg weekly | Every 4 weeks | 2.4 mg weekly 19 |
Tirzepatide (Zepbound) | 2.5 mg weekly | Every 4 weeks | 5 mg to 15 mg weekly 19 |
Liraglutide (Saxenda) | 0.6 mg daily | Every 1 week | 3.0 mg daily 22 |
For patients who have reached the maximum dose of a single-hormone agonist like semaglutide but have plateaued, switching to a dual-incretin therapy like tirzepatide may be effective.2 Tirzepatide acts on both GLP-1 and GIP receptors, providing a synergistic effect that further suppresses appetite and improves metabolic markers beyond what GLP-1 alone can achieve.2 GIP signaling is believed to enhance the body’s sensitivity to GLP-1 while also potentially modifying adipocyte metabolism to favor fat oxidation.2
Adjunctive Pharmacotherapy and Combination Treatments
In some cases, the addition of a second anti-obesity medication is necessary to overcome significant metabolic resistance.11 The combination of a GLP-1 RA with phentermine, a sympathomimetic amine that stimulates norepinephrine release to suppress appetite, has been used clinically to “jumpstart” weight loss during a plateau.26 Similarly, the combination of phentermine and topiramate (Qsymia) can be used as an adjunct.27 Topiramate, an anti-epileptic medication, is thought to promote satiety and reduce cravings through GABAergic modulation and glutamate antagonism.28
Adjunctive Strategy | Mechanism of Action | Clinical Application |
GLP-1 + Phentermine | Dual central appetite suppression via incretin and catecholamine pathways.26 | Used for short-term (12-week) intervention to break plateaus.26 |
GLP-1 + SGLT2 Inhibitor | Improved glycemic control and caloric excretion through urine.6 | Beneficial for patients with comorbid type 2 diabetes or heart failure.11 |
GLP-1 + Metformin | Sensitization to insulin and modest appetite suppression.6 | Often used as a foundational therapy in metabolic syndrome.11 |
The “Muscle Floor” and Resistance Training
A critical and often overlooked factor in weight loss plateaus is the loss of lean muscle mass.11 Rapid weight loss on GLP-1 RAs can result in a significant portion of the loss coming from muscle rather than fat—estimates suggest up to 40% in some populations.12 Muscle tissue is more metabolically active than adipose tissue; thus, the loss of muscle further depresses the BMR, making continued weight loss nearly impossible.7
The body may reach a “muscle floor,” where it resists further weight loss to prevent the depletion of essential lean mass.32 To counter this, patients must prioritize resistance training two to three times per week and ensure an adequate intake of high-quality protein (typically 0.8 to 1.2 grams per kilogram of body weight).11 Preserving or building muscle mass helps maintain a higher BMR and can “re-prime” the metabolism to resume fat loss.13
Advanced Dosing Schedules and Off-Label Dosing Intervals
As weight loss stalls, some clinical protocols and patient-led initiatives have explored the modification of the standard seven-day dosing interval.34 The most common adjustment is shortening the interval to an injection every six days.34
Pharmacokinetic Rationale for Six-Day Dosing
The pharmacokinetics of the most common weekly GLP-1 RAs are governed by their relatively long half-lives: semaglutide has a half-life of approximately seven days (168 hours), and tirzepatide has a half-life of approximately five days (120 hours).20 These long durations of action are achieved through molecular modifications that enhance stability and reduce renal clearance, allowing the medication to reach a “steady state” in the body after four to five weeks of regular dosing.21
Steady state represents a dynamic equilibrium where the amount of drug administered equals the amount eliminated between doses.38 In a standard seven-day cycle, the plasma concentration of the medication reaches its peak () within one to three days post-injection and then declines to its trough level () by day seven.20 Shortening the interval to six days effectively increases the accumulation factor of the medication.38
The accumulation factor () is determined by the formula:
where is the elimination rate constant () and is the dosing interval.38 By reducing from seven days to six days, the average concentration () and the trough concentration () are raised.39 Clinically, this is intended to prevent the “wear-off” effect often reported by patients toward the end of their weekly cycle, where appetite suppression wanes as the drug concentration approaches the trough.1
The Side Effects of Increased Dosing Frequency
Increasing the frequency of GLP-1 RA injections to every six days is an off-label practice that significantly alters the drug’s safety profile.15 The side effects of these medications are profoundly dose-dependent, and shortening the interval results in higher sustained concentrations and higher peaks than those validated in clinical trials.3
Intensified Gastrointestinal Distress
The most frequent adverse effects—nausea, vomiting, diarrhea, and constipation—are largely mediated by the slowing of gastric motility and the activation of satiety centers in the brain.9 A six-day dosing schedule can overwhelm the body’s ability to adapt to these effects.17 Patients who were stable on a seven-day schedule may experience a resurgence of severe nausea or vomiting as the steady-state concentration rises.41 In extreme cases, this can lead to clinical gastroparesis, where gastric emptying is slowed to a degree that compromises nutritional intake and hydration.44
Risk of Dehydration and Renal Injury
Chronic vomiting and diarrhea associated with high-dose GLP-1 therapy can lead to rapid volume depletion.20 Dehydration is a primary cause of acute kidney injury (AKI) in this patient population.41 Shortening the dosing interval increases the likelihood of persistent gastrointestinal distress, thereby escalating the risk of renal complications.20 Clinicians often monitor renal function and electrolytes closely in patients who deviate from standard dosing schedules.5
Cardiovascular and Endocrine Considerations
GLP-1 RAs are known to cause a mild increase in resting heart rate, typically 2 to 4 beats per minute.41 Escalating the dose frequency may lead to more pronounced tachycardia or palpitations, which can be distressing for patients with underlying cardiac conditions.26 Additionally, while GLP-1 RAs have a low risk of hypoglycemia when used alone, the risk increases significantly if the dose is concentrated or if the patient is also taking insulin or sulfonylureas.20
Adverse Effect | Mechanism in 6-Day Dosing | Severity/Risk Level |
Nausea/Vomiting | Peak concentration () exceeds the adaptive threshold of the area postrema.17 | High; may lead to treatment discontinuation.3 |
Diarrhea | Altered bowel transit time and changes in gut microbiota signaling.41 | Moderate; increases risk of dehydration.20 |
Acute Kidney Injury | Secondary to severe volume contraction from GI side effects.20 | Rare but Severe; requires immediate medical intervention.42 |
Tachycardia | Heightened sympathetic activation or direct effect on sinoatrial node receptors.41 | Low to Moderate; necessitates cardiovascular monitoring.26 |
Gastroparesis | Profound inhibition of gastric motility beyond therapeutic intent.44 | Rare; may require hospitalization and bowel rest.44 |
The Role of Lifestyle Factors in Plateau Management
While pharmacological adjustments are often the focus of plateau management, lifestyle factors such as sleep, stress, and behavioral consistency are equally critical in determining long-term outcomes.6
Sleep, Stress, and Cortisol
Chronic sleep deprivation and high levels of stress are potent inhibitors of weight loss, even on GLP-1 medications.6 Poor sleep disrupts the balance of hunger hormones, increasing ghrelin and decreasing leptin, which can bypass the appetite-suppressing effects of the medication.6 Stress triggers the release of cortisol, which promotes the storage of visceral fat and increases cravings for calorie-dense foods.6 Managing these factors is often a prerequisite for breaking a plateau that appears resistant to medication adjustments.11
Behavioral Drift and “Hidden” Calories
Over time, patients may experience behavioral drift, where the dietary habits established at the beginning of treatment begin to loosen.7 Small increases in portion sizes, the reintroduction of liquid calories, or frequent snacking can add up to enough calories to offset the metabolic slowdown, resulting in a weight stall.11 Brief periods of food logging or meeting with a registered dietitian can help patients identify these “hidden” calories and realign their intake with their new, lower energy requirements.11
Pharmacokinetic Modeling of Alternative Regimens: A Comparative View
The decision to modify a dosing regimen must be grounded in an understanding of how frequency changes affect the steady-state concentration and the therapeutic window.17
Comparison of Weekly vs. Bi-Weekly vs. Monthly Efficacy
Recent mathematical modeling of semaglutide and tirzepatide has investigated the relationship between dosing frequency and weight loss retention.39 These models reveal a non-linear relationship between the amount of drug administered and the biological response.39
For example, reducing the dosing frequency from once-weekly to once every two weeks (effectively halving the total drug amount over time) does not result in a 50% reduction in efficacy.39 Instead, patients retain approximately 72% to 75% of their weight loss.39 This suggests that the body’s response to higher or more frequent doses eventually reaches a point of diminishing returns, where additional drug increases the risk of side effects significantly more than it increases weight loss.15
Dosing Frequency (2.4mg Semaglutide) | Total Monthly Drug | Predicted Weight Loss Retention | Accumulation Variability (Cmax−Cmin) |
Once Weekly (q1wk) | 9.6 mg | 100% (Baseline) | Standard 39 |
Once Every 2 Weeks (q2wk) | 4.8 mg | ~72% | Increases by 34% 39 |
Once Monthly (q4wk) | 2.4 mg | ~50% | Significant Peak/Trough gaps 39 |
Every 6 Days (q6d) | ~11.2 mg | ~105-110% | Decreases variability, increases 38 |
The “Steady State” Equilibrium
Reaching steady state is crucial because it ensures consistent appetite regulation throughout the week.21 When the dosing interval is shortened to six days, the body reaches a new, higher steady state.38 While this may suppress late-cycle hunger, it also increases the risk of receptor saturation, where all available GLP-1 receptors are occupied, and further increases in drug concentration provide no additional therapeutic benefit—only additional toxicity.15
Comprehensive Management Framework for the Plateaued Patient
Managing a weight loss plateau in GLP-1 therapy requires a systematic approach that addresses the biological, pharmacological, and behavioral drivers of stagnation.
Phase 1: Re-Evaluation and Diagnostics
The initial step is to confirm the existence of a true plateau (weight stability for >4 weeks) and rule out secondary medical causes.4 Clinicians may perform metabolic testing, such as measuring the Resting Metabolic Rate (RMR) or using DEXA scans to assess body composition changes.13 Laboratory evaluations for thyroid function (TSH), cortisol levels, and sex hormones (testosterone, estrogen) can identify hormonal imbalances that may be contributing to the stall.10
Phase 2: Nutritional and Exercise Optimization
Before adjusting medication, the foundational pillars of weight management must be optimized.11 This includes:
- Protein Prioritization: Ensuring the patient consumes 1.2g/kg of protein to preserve the BMR.18
- Resistance Training: Implementing a progressive strength program to counteract adaptive thermogenesis.13
- Fiber and Hydration: Managing constipation and ensuring satiety through whole-food volume and adequate water intake.12
Phase 3: Pharmacological Intervention
If lifestyle optimization is insufficient, pharmacological adjustments are introduced:
- Titration to Max Dose: Completing the standard escalation to 2.4 mg (semaglutide) or 15 mg (tirzepatide).3
- Switching Agents: Transitioning from a GLP-1 RA to a dual GLP-1/GIP RA to leverage synergistic pathways.2
- Combination Therapy: Adding phentermine or topiramate for dual-mechanism appetite control.26
- Dosing Frequency Modification: As a final, off-label step, some clinicians may consider shortening the interval to six days, while providing intensive counseling on the risks of GI distress and dehydration.38
The Future of Obesity Management and the Plateau
As the clinical understanding of GLP-1 and other incretin-based therapies evolves, the goal of treatment is shifting from rapid weight loss to sustainable metabolic health.9 Emerging therapies, such as the triple agonist retatrutide (targeting GLP-1, GIP, and glucagon receptors), aim to bypass current plateaus by further increasing metabolic rate and fat oxidation.2
However, for the majority of patients, the plateau is an inevitable part of the journey—a signal that the body has successfully adjusted to a lower energy state.1 Recognizing this adaptation as a physiological milestone rather than a clinical failure allows for a more rational and empathetic approach to long-term obesity management.1 The “chronic disease” model of obesity implies that management will be lifelong, involving the titration and maintenance of pharmacological tools alongside the preservation of the body’s metabolic machinery.9
In summary, weight loss plateaus are driven by the body’s homeostatic defense mechanisms, primarily metabolic adaptation, hormonal shifts, and pharmacological receptor desensitization.1 Strategies to overcome these stalls include maximizing medication doses, switching to dual-agonist therapies, prioritizing resistance training for muscle preservation, and addressing environmental inhibitors such as poor sleep and high stress.2 While advanced dosing strategies like a six-day injection interval may raise steady-state drug levels to suppress lingering hunger, they must be balanced against a significant risk of intensified gastrointestinal side effects and potential renal complications.17
Works cited
- Why GLP-1 Plateaus Happen and How Telehealth Programs …, accessed May 10, 2026, https://www.how-dept.com/mayiknow/detail/?p=Why-GLP-1-Plateaus-Happen-and-How-Telehealth-Programs-Address-Them-AvGMFw9N72X9k
- Semaglutide Plateauing? Overcoming Stalled Weight Loss by Switching – Drip Gym, accessed May 10, 2026, https://dripgym.com/blogs/news/semaglutide-weight-loss-plateau-switching-options
- Evaluating Dose Titration in Semaglutide and Tirzepatide for Weight Loss: A Retrospective Academic Call Center Study – MDPI, accessed May 10, 2026, https://www.mdpi.com/2673-4168/5/4/90
- GLP-1 Plateau: Why You Stopped Losing Weight and What to Do – Doctronic, accessed May 10, 2026, https://www.doctronic.ai/blog/glp-1-plateau/
- How to Break a Weight Loss Plateau with GLP-1 Therapy – Harmony Aesthetics Medical Spa, accessed May 10, 2026, https://harmonyaestheticsspa.com/how-to-break-a-weight-loss-plateau/
- What To Do If You Plateau On A GLP-1 Medication – Spruce Aesthetics + Infusion Bar, accessed May 10, 2026, https://sprucespa.com/what-to-do-if-you-plateau-on-a-glp-1-medication/
- Why You’re Hitting a Weight-Loss Plateau on Semaglutide (and What to Do About It) – Greenwich Medical Spa, accessed May 10, 2026, https://www.greenwichmedicalspa.com/blog/why-youre-hitting-a-weight-loss-plateau-on-semaglutide-and-what-to-do-about-it/
- Metabolic Adaptation | Rethink Obesity®, accessed May 10, 2026, https://www.rethinkobesity.com/obesity-disease/metabolic-adaptation.html
- GLP-1 Balanced: How to Maintain Results Long Term, accessed May 10, 2026, https://revistas.ucatolicaluisamigo.edu.co/plugins/generic/pdfJsViewer/pdf.js/web/viewer.html?file=%2Findex.php%2Findex%2Flogin%2FsignOut%3Fsource%3D%2Egifx7%2Ecom&io0=ctrnbcxbg1jh
- How Do I Break a Weight Loss Plateau? Understanding Metabolic Set Points – Blue Sky MD, accessed May 10, 2026, https://blueskymd.com/how-do-i-break-a-weight-loss-plateau-understanding-metabolic-set-points/
- Frustrated by GLP-1? Why Weight Stalls & Medically Approved Next Steps | Ubie Doctor’s Note, accessed May 10, 2026, https://ubiehealth.com/doctors-note/glp1-frustrated-weight-stalls-medics-next-steps-4723e2
- Weight Loss Stalling While on GLP-1s – Torrance Memorial, accessed May 10, 2026, https://www.torrancememorial.org/healthy-living/blog/weight-loss-stalling-while-on-glp-1s/
- Tips for Overcoming a Weight-Loss Plateau – Banner Health, accessed May 10, 2026, https://www.bannerhealth.com/healthcareblog/advise-me/how-to-get-over-your-weight-loss-plateau
- How to Overcome Weight Loss Plateaus With GLP-1 – Sota Wellness, accessed May 10, 2026, https://sotawellness.com/blog/strategies-and-tips-for-overcoming-weight-loss-plateaus-with-glp-1-medications/
- GLP-1 Microdosing for Weight Loss: Pros and Cons | Paloma Health, accessed May 10, 2026, https://www.palomahealth.com/learn/glp-1-microdosing-weight-loss-pros-cons
- How to Safely Restart GLP-1 Medications After a Break | Mochi Health, accessed May 10, 2026, https://joinmochi.com/blogs/how-to-restart-after-taking-a-break-from-glp-1s
- GLP-1 Microdosing Chart: How GLP Activate Supports Your Journey, accessed May 10, 2026, https://cuaderno.pucmm.edu.do/plugins/generic/pdfJsViewer/pdf.js/web/viewer.html?file=%2Findex.php%2Findex%2Flogin%2FsignOut%3Fsource%3D%2Egifx7%2Ecom&io0=t7of2cxp6koo
- Stalled on Tirzepatide? Why Your Body Plateaus & Approved Medical Steps | Ubie Doctor’s Note, accessed May 10, 2026, https://ubiehealth.com/doctors-note/tirzepatide-stalled-plateau-body-approved-steps-4223e2
- GLP-1 Dose Adjustment for Weight Loss: When to Adjust – Healthline, accessed May 10, 2026, https://www.healthline.com/health/drugs/glp-1-dose-adjustment-for-weight-loss
- Semaglutide – StatPearls – NCBI Bookshelf, accessed May 10, 2026, https://www.ncbi.nlm.nih.gov/books/NBK603723/
- Half-Life of Mounjaro: Dosing, Duration and Clinical Implications …, accessed May 10, 2026, https://www.boltpharmacy.co.uk/guide/half-life-of-mounjaro
- A Comprehensive Review on the Pharmacokinetics and Drug−Drug Interactions of Approved GLP-1 Receptor Agonists and a Dual GLP-1/GIP Receptor Agonist – PMC, accessed May 10, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12052016/
- UPDATES to the GLP1-RA Dose Comparisons Chart, accessed May 10, 2026, https://www.wafp.org/assets/files/pdfs/GLP%20equivalent%20Doses%20UPDATED%20chart.pdf
- Tirzepatide modulates the regulation of adipocyte nutrient metabolism through long-acting activation of the GIP receptor | Request PDF – ResearchGate, accessed May 10, 2026, https://www.researchgate.net/publication/381442121_Tirzepatide_modulates_the_regulation_of_adipocyte_nutrient_metabolism_through_long-acting_activation_of_the_GIP_receptor
- (PDF) Chronic glucose-dependent insulinotropic polypeptide receptor (GIPR) agonism desensitizes adipocyte GIPR activity mimicking functional GIPR antagonism – ResearchGate, accessed May 10, 2026, https://www.researchgate.net/publication/345315409_Chronic_glucose-dependent_insulinotropic_polypeptide_receptor_GIPR_agonism_desensitizes_adipocyte_GIPR_activity_mimicking_functional_GIPR_antagonism
- Why Combine Phentermine and GLP-1? Understanding This Powerful Weight Loss Strategy, accessed May 10, 2026, https://www.valleymedicalweightloss.com/blog/why-combine-phentermine-and-glp-1/
- Phentermine and topiramate (oral route) – Side effects & dosage – Mayo Clinic, accessed May 10, 2026, https://www.mayoclinic.org/drugs-supplements/phentermine-and-topiramate-oral-route/description/drg-20075700
- Topiramate and phentermine for weight loss: Is it effective? – Healthline, accessed May 10, 2026, https://www.healthline.com/health/drugs/topiramate-and-phentermine
- How to Take Qsymia for Weight Loss: Dos And Don’ts – GoodRx, accessed May 10, 2026, https://www.goodrx.com/qsymia/how-to-take
- Diabetes Drugs by Class, accessed May 10, 2026, https://www.wwhealth.org/wp-content/uploads/2016/05/I.-Meds-reduced-2021_reduced.pdf
- US20240390464A1 – Treatment of Adults With Overweight or Obesity With or Without Weight-Related Comorbidities – Google Patents, accessed May 10, 2026, https://patents.google.com/patent/US20240390464A1/en
- Stopping and restarting certain GLP-1s to lose weight may make the drug less effective, accessed May 10, 2026, https://www.pennmedicine.org/news/stopping-and-restarting-glp1s-may-make-it-less-effective
- Maintenance Dosing with Tirzepatide and Semaglutide: What the data tells us., accessed May 10, 2026, https://levesqueplasticsurgery.com/blog/maintenance-dosing-with-tirzepatide-and-semaglutide-whats-the-data-tells-us
- acting GLP-1 receptor agonist, exendin-4–Fc fusion – RSC Publishing, accessed May 10, 2026, https://pubs.rsc.org/en/content/articlepdf/2017/ra/c7ra10822b
- In vitro and in vivo characterization of a novel long-acting GLP-1 receptor agonist, exendin-4–Fc fusion protein – RSC Publishing, accessed May 10, 2026, https://pubs.rsc.org/en/content/articlehtml/2017/ra/c7ra10822b
- US11707610B2 – Ingestible device for delivery of therapeutic agent to the gastrointestinal tract – Google Patents, accessed May 10, 2026, https://patents.google.com/patent/US11707610B2/en
- INGESTIBLE DEVICE FOR DELIVERY OF THERAPEUTIC AGENT TO THE GASTROINTESTINAL TRACT – European Patent Office – EP 4309722 A2 – Googleapis.com, accessed May 10, 2026, https://patentimages.storage.googleapis.com/48/f3/bf/5e64a5d5a8a90d/EP4309722A2.pdf
- Does GLP-1 Build Up in Your System? Understanding Steady State – Bolt Pharmacy, accessed May 10, 2026, https://www.boltpharmacy.co.uk/guide/does-glp-1-build-up-in-your-system
- Alternative dosing regimens of GLP‐1 receptor agonists may reduce …, accessed May 10, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11885104/
- Microdosing GLP-1s: Does It Work? Risks and Benefits – GoodRx, accessed May 10, 2026, https://www.goodrx.com/conditions/weight-loss/microdosing-glp-1
- Glucagon-Like Peptide-1 Receptor Agonists – StatPearls – NCBI Bookshelf, accessed May 10, 2026, https://www.ncbi.nlm.nih.gov/books/NBK551568/
- GLP-1 Agonists – Cleveland Clinic, accessed May 10, 2026, https://my.clevelandclinic.org/health/treatments/13901-glp-1-agonists
- Missed GLP-1 Dose: What happens, what to do, and how to prevent it – Healthline, accessed May 10, 2026, https://www.healthline.com/health/drugs/missed-glp-1-dose
- Oral Semaglutide for Weight Loss: Key Facts About the Wegovy Pill – GoodRx, accessed May 10, 2026, https://www.goodrx.com/conditions/weight-loss/oral-semaglutide-weight-loss
- Switching between weight-loss medications – The Pharmaceutical Journal, accessed May 10, 2026, https://pharmaceutical-journal.com/article/ld/switching-between-weight-loss-medications
- Clinical Pharmacokinetics of Semaglutide: A Systematic Review – PMC, accessed May 10, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11215664/
- Use of a GLP-1R Agonist to Treat Opioid Use Disorder NCT number: NCT04199728 Docume – ClinicalTrials.gov, accessed May 10, 2026, https://cdn.clinicaltrials.gov/large-docs/28/NCT04199728/Prot_SAP_000.pdf