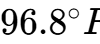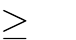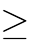The Neuro-Clinical Frontier: A Comprehensive Analysis of Near-Death Experiences and the Evolution of Death by Neurologic Criteria
The determination of the precise moment of death has undergone a profound transformation over the last century, moving from a primarily cardiopulmonary observation to a sophisticated neurological evaluation. This shift has created a complex intersection between the medical-legal definition of death by neurologic criteria (BD/DNC) and the subjective phenomena of near-death experiences (NDEs). As resuscitation techniques have advanced, allowing for the restoration of life in patients who were previously considered unsalvageable, a growing body of empirical research has emerged to investigate the nature of consciousness during these physiological crises. This report examines the evolution of brain death standards, the rigorous categorization of NDEs, and the latest neurobiological research over the last twenty years that seeks to correlate these profound experiences with the physiological state of the dying brain.
Medical and Legal Foundations of Death by Neurologic Criteria
The legal framework for death in the United States and much of the industrialized world is rooted in the dual-criteria model established by the Uniform Determination of Death Act (UDDA) of 1980.1 This act stipulates that an individual is dead if they have sustained either the irreversible cessation of circulatory and respiratory functions or the irreversible cessation of all functions of the entire brain, including the brainstem.2 The latter, commonly referred to as brain death or death by neurologic criteria (DNC), remains a subject of intense clinical scrutiny to ensure that the declaration of death is absolute and beyond error.5
The 2023 Revised Consensus Guidelines for BD/DNC
In October 2023, a critical advancement in the standardization of death determination occurred with the publication of the revised consensus practice guideline in the journal Neurology.7 This document, authored by Greer et al., represents the first time that guidance for both adults and children has been integrated into a single, comprehensive framework.7 The integration was necessary because previous standards varied significantly between age groups and institutions, leading to potential legal ambiguities and a loss of public trust in the medical system.5
The 2023 guidelines maintain that BD/DNC occurs in individuals who have sustained a catastrophic and permanent brain injury, with no evidence of the function of the brain as a whole.4 The determination rests on a standardized procedure that requires three essential findings: unresponsive coma, the absence of brainstem areflexia, and apnea.1
Prerequisites and Confounder Mitigation
Before a clinician can initiate a BD/DNC evaluation, several stringent prerequisites must be met to ensure the observed unresponsiveness is not due to reversible factors. The injury must be catastrophic and the mechanism known, such as a severe traumatic brain injury, massive subarachnoid hemorrhage, or hypoxic-ischemic insult following cardiac arrest.1 Clinicians are required to rule out and correct any confounding conditions that might mimic brain death, including severe electrolyte imbalances, metabolic derangements, or acid-base disturbances.2
Parameter | Required Standard for BD/DNC Evaluation | Clinical Rationale |
Core Temperature |
| Prevent hypothermic suppression of brain function 4 |
Systolic Blood Pressure | Adult: | Ensure adequate cerebral perfusion during testing 2 |
Drug Clearance |
| Eliminate pharmacological effects on consciousness 4 |
Metabolic State | Correction of severe hypo/hypernatremia, hypo/hyperglycemia | Rule out reversible metabolic coma 2 |
For pediatric patients, the requirements are even more conservative. For children younger than 24 months, clinicians must wait at least 48 hours after the initial brain injury before commencing an evaluation.2 The revised guidelines also standardize the interval between the two required neurologic examinations and apnea tests in children to a minimum of 12 hours, regardless of age.7
The Clinical Neurological Examination
The 2023 guidelines emphasize that BD/DNC is fundamentally a clinical assessment.12 The examination involves a systematic head-to-toe evaluation of brainstem reflexes, ensuring that no cerebrally mediated motor responses exist.4
- Assessment of Unresponsiveness: The patient must be completely comatose and unresponsive to all visual, auditory, and tactile stimuli.4
- Brainstem Areflexia: Clinicians test for the absence of several key reflexes. This includes the pupillary light reflex (cranial nerves II and III), the corneal reflex (V and VII), the oculocephalic and oculovestibular reflexes (III, VI, and VIII), and the gag and cough reflexes (IX and X).2
- Apnea Testing: This is the final step in the clinical evaluation, designed to determine if the brainstem has lost the capacity for spontaneous respiratory drive. The patient is challenged with a rise in
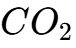 and a corresponding drop in
and a corresponding drop in 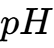 (acidosis) to provide a maximal stimulus for breathing.2 If no respiratory effort is observed despite an adequate stimulus, typically a
(acidosis) to provide a maximal stimulus for breathing.2 If no respiratory effort is observed despite an adequate stimulus, typically a 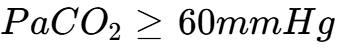 or
or 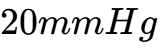 above baseline, the apnea test is considered positive.2
above baseline, the apnea test is considered positive.2
If the clinical exam cannot be completed—due to ocular trauma, severe facial injury, or instability during the apnea test—ancillary tests such as SPECT radionuclide perfusion scintigraphy or 4-vessel catheter angiography are required to confirm the absence of cerebral blood flow.2
Taxonomy and Phenomenology of Near-Death Experiences
Near-death experiences are vivid, realistic, and subjective episodes that typically occur during life-threatening crises such as cardiac arrest, trauma, or coma.15 Over the last twenty years, researchers have moved away from viewing these as mere hallucinations, instead treating them as a specific class of altered states of consciousness with consistent cross-cultural themes.16
The Greyson NDE Scale and Systematic Classification
To provide a rigorous framework for identifying NDEs, the Greyson NDE Scale remains the gold standard. Developed by Bruce Greyson in 1983, the 16-item scale quantifies the depth of the experience across four dimensions: cognitive, affective, paranormal, and transcendental.19 A score of 7 or higher identifies an individual as a "near-death experiencer" (NDEr).19
Dimension | Characteristic Elements | Descriptive Features |
Cognitive | Time distortion, thought acceleration, life review | A sense that time loses meaning; re-experiencing life events as a panoramic movie 15 |
Affective | Peace, joy, cosmic unity, unconditional love | Disappearance of pain; a feeling of belonging to a larger whole 15 |
Paranormal | Out-of-body experience (OBE), extrasensory perception | Seeing the physical body from a detached vantage point; awareness of distant events 15 |
Transcendental | Being of light, deceased relatives, other realms | Entering a tunnel toward a brilliant light; meeting sentient "entities" or religious figures 15 |
Cultural Variations in Phenomenology
While the "core experience" of an NDE is remarkably consistent worldwide, cultural and religious backgrounds influence the specific symbols and descriptions used by experiencers.16 In Western accounts, the experience frequently begins with a tunnel and a sense of movement toward a light.15 However, research into non-Western cases has revealed intriguing differences. For example, in Thai NDEs, tunnels are rarely reported; instead, the experience often begins with an encounter with "Yamatoots" (messengers of death in Hinduism and Buddhism).15 Similarly, while Christians may report seeing Jesus Christ, Shīʿī Muslims often identify religious figures as Shiite imams.15
Maori case studies have identified that while the narratives include traditional "common core" features like OBEs and heightened senses, the interpretation of the "other realm" is deeply rooted in indigenous spirituality.15 These findings suggest that while the biological mechanism of the NDE may be universal, the brain interprets the experience through the lens of the individual's cultural and personal expectations.15
The Darker Spectrum: Distressing Near-Death Experiences
Although the majority of NDEs are characterized by feelings of immense peace and love, a significant minority—estimated at 1% to 10%—are distressing or even terrifying.15 These experiences challenge the "expectancy model," which suggests that NDEs are merely pleasurable fantasies constructed to protect the individual from the shock of death.16
Typologies of Distressing NDEs
Researchers have documented three primary types of distressing NDEs, each with unique psychological characteristics.24
- The Inverse NDE: In this type, the experiencer encounters typical NDE elements but perceives them with hostility or panic. A person may find themselves floating above their body and feel a desperate, terrifying loss of control, screaming to be put back.24 The "bright light" that others find comforting may be perceived as a blinding, aggressive force on a collision course.24
- The Void NDE: This is characterized by an ontological encounter with a vast, empty space—a devastating sense of aloneness and isolation.24 Individuals may report being told they "never existed" and that their entire life was a joke, leaving them in a state of eternal annihilation.24
- The Hellish NDE: These are the rarest and involve overtly hellish imagery. Accounts include falling into pits or being taken to gates of rust, encounters with malevolent beings with gray appendages, or seeing lost spirits in pain.24 Experiencers may report the "indescribable stench" of these realms and the "gnashing of teeth".24
Despite their distressing nature, these experiences can have transformative effects. One case study involves a 25-year-old woman who, after surviving a traumatic brain injury and a distressing NDE, reported the complete resolution of her pre-accident suicidal ideation, viewing the experience as a profound psychological "reset".25
Landmark Research of the Last Two Decades: The AWARE Studies
The most significant progress in correlating near-death experiences with the physiological state of the brain has come from prospective multi-center studies, most notably the AWAreness during REsuscitation (AWARE) projects led by Dr. Sam Parnia.
AWARE I: Investigating the Incidence of Awareness
Launched in 2008, the first AWARE study followed 2,060 cardiac arrest patients across 15 medical centers in the United Kingdom, United States, and Austria.26 This study was the first large-scale effort to objectively test the validity of conscious experiences using hidden visual markers in resuscitation rooms.27
The results showed that 39% of cardiac arrest survivors reported a perception of awareness despite showing no clinical evidence of consciousness at the time.26 While only 9% had experiences compatible with the classic NDE, 2% reported full awareness with explicit recall of seeing and hearing events during their resuscitation.27 One particularly significant case involved a patient who accurately described the auditory stimuli and activities of medical personnel for a three-minute period during which he had no heartbeat.27 This finding was paradoxical, as the brain typically ceases functioning within 20 to 30 seconds of the heart stopping.27
AWARE II: EEG Biomarkers of Consciousness During CPR
The AWARE II study, published in 2023, sought to analyze the relationship between brain function and awareness during cardiac arrest and resuscitation using real-time electroencephalography (EEG) and cerebral oximetry (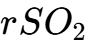 ).26 The study monitored 567 in-hospital cardiac arrests across 25 sites.29
).26 The study monitored 567 in-hospital cardiac arrests across 25 sites.29
The most striking finding of AWARE II was the emergence of normal EEG activity (delta, theta, and alpha waves) in patients as long as 35 to 60 minutes into CPR.29 These rhythms, consistent with a resumption of network-level cognitive activity, emerged despite marked cerebral ischemia (mean 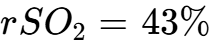 ).29 Researchers identified a specific category of experience termed "Transcendent Recalled Experience of Death" (RED), which occurred in 21.4% of interviewed survivors.29 This study suggests that the brain may undergo a period of "disinhibition" during death—the removal of normal inhibitory filters—allowing for a surge of lucidity and complex internal consciousness just as external responsiveness ceases.30
).29 Researchers identified a specific category of experience termed "Transcendent Recalled Experience of Death" (RED), which occurred in 21.4% of interviewed survivors.29 This study suggests that the brain may undergo a period of "disinhibition" during death—the removal of normal inhibitory filters—allowing for a surge of lucidity and complex internal consciousness just as external responsiveness ceases.30
Study Characteristic | AWARE I (2008-2014) | AWARE II (2023) |
Patient Population | 2,060 cardiac arrest events 28 | 567 in-hospital cardiac arrests 29 |
Primary Method | Structured interviews; hidden visual targets 26 | Real-time EEG; cerebral oximetry during CPR 29 |
Key Findings | 39% perception of awareness; 2% explicit OBE 27 | Normal EEG activity 35-60 mins into CPR; RED identified 29 |
Consciousness Type | Explicit and implicit memory recall 26 | Biomarkers of "disinhibited" cortical activity 29 |
Neurobiological Mechanisms and Theories of the Dying Brain
Contemporary research has proposed several physiological models to explain how the dying brain might generate the vivid content of an NDE. These models range from ischemic stress and gas exchange to complex neurochemical surges.
The G-LOC Model and Ischemic Stress
Studies of fighter pilots undergoing high-speed centrifugal acceleration (+Gz stress) provide a compelling analog for NDEs.31 This stress causes blood to pool in the lower body, leading to rapid cerebral hypotension and cephalic ischemia.31 Pilots experiencing G-induced loss of consciousness (G-LOC) frequently report extraordinary perceptions that occur within seconds, including tunnel vision, floating sensations, and dream-like vignettes.31 The overlap between G-LOC themes and original NDE reports suggests that a temporarily reduced blood flow to the brain is a sufficient trigger for many NDE features.31
Anoxic Depolarization and the "Wave of Death"
The "wave of death" is a paradoxical surge in brain electrical activity that has been observed at the point of death in both animals and humans.14 As the heart stops, the brain initially shuts down, followed by a sudden burst of high-frequency gamma and beta waves.14 This activity is associated with anoxic depolarization—a massive release of ionic energy as neurons lose the ability to maintain their electrochemical gradients.14 While some believe this reflects a final recall of life, critics argue that these waves are often contaminated by muscle artifacts (electromyographic activity) and may not represent coherent cognitive processing.33
Neurochemistry: The DMT and Serotonergic Hypotheses
N,N-Dimethyltryptamine (DMT), a potent serotonergic psychedelic, has become a central focus of NDE neurochemistry. Research has shown that DMT-induced experiences frequently reach the Greyson NDE Scale threshold for a "true" NDE, featuring out-of-body sensations, encounters with non-physical entities, and the perception of a transcendental realm.21
Recent animal studies have confirmed the presence of endogenous DMT in various cortical sites at levels comparable to serotonin and dopamine, suggesting it may act as a neurotransmitter that modulates perception during extreme physiological crises.35 Furthermore, DMT administration causes dose-dependent increases in serotonin and dopamine, along with increased gamma functional connectivity, which may provide the neurochemical substrate for the heightened alertness and clarity reported by NDErs.34
Biophotons and Visual Phosphenes
A novel biophysical model suggests that the "brilliant light" of NDEs arises from reperfusion injury following ischemia.36 The unregulated overproduction of free radicals during reperfusion can generate energetically excited molecules that release bioluminescent biophotons.36 If this photon emission exceeds a certain threshold in the retinotopic visual areas of the brain, the individual perceives them as intense external lights (phosphenes).36 This suggests that the visual hallmark of the NDE has a direct basis in the quantum biophysics of the dying cell.
Case Studies and the Evidence of Veridical Perception
The most controversial aspect of NDE research is "veridical perception"—reports of accurate observations of the material world that the individual could not have obtained through normal sensory means while unconscious.23
The Case of Pam Reynolds (1991) and Modern Critiques
The Pam Reynolds case is often cited as the most significant documented NDE.38 During a specialized "standstill" surgery to repair a giant basilar aneurysm, Reynolds was rendered clinically dead: her heart was stopped, her brain was drained of blood, and her eyes were taped shut while speakers in her ears emitted loud, rapid clicks to monitor her brainstem function.38 Despite having a flat electroencephalogram (EEG), Reynolds later reported an out-of-body experience where she observed the surgical saw (which she correctly described as looking like an electric toothbrush) and heard the surgical team discuss the diameter of her blood vessels.38
Critics have offered more prosaic explanations, such as "anesthesia awareness," where the patient may have heard sounds or felt sensations during the hours of surgery before or after the period of hypothermic cardiac arrest.38 Others point to the fact that the clicking sounds in her ears might not have been loud enough to block out all external noise, or that her traumatic brain injury may have idiosyncratically influenced her EEG recording.33
Lloyd Rudy and the Verification of "Eyeless Vision"
In contrast to the critiques of older cases, the report by cardiac surgeon Lloyd Rudy provides a more recent account of veridical perception confirmed by objective observers.42 Rudy reported a case where a patient, during a period of prolonged flat-line ECG and EEG activity, accurately perceived phenomena in the operating room that were later confirmed by Rudy’s assistant surgeon.42 This case is noted for its level of third-party verification, which remains a key requirement for any claim of veridicality.42
A significant development in this field is the creation of the Veridical Near-Death Experience (vNDE) Scale, introduced in 2025 to evaluate the evidential strength of such reports.23 In trials using 17 potential cases, independent human raters and artificial intelligence models (LLMs) achieved high agreement in categorizing the strength of evidence, providing a more objective tool for investigating these anomalous accounts.43
Evaluating the Correlation Between BD/DNC and NDEs
The ultimate question in this field is whether a patient who meets the clinical criteria for brain death (BD/DNC) can experience a near-death experience. This requires distinguishing between clinical death (reversible cessation of circulation) and brain death (irreversible cessation of all brain function).1
The Medical-Legal Consensus vs. Subjective Reports
From a medical-legal perspective, the American Academy of Neurology (AAN) asserts that there are no known cases where a patient who met the standard BD/DNC guidelines subsequently recovered consciousness.12 BD/DNC is considered "final and cannot be reversed".3 By this definition, if a person reports an NDE, they were never truly brain dead; rather, they experienced a state of clinical death from which they were resuscitated.18
However, the discovery of "covert consciousness"—also known as Cognitive Motor Dissociation (CMD)—has introduced a "gray zone" into this debate.14 CMD is a state where a patient shows no behavioral response to commands but demonstrates willful modulation of brain activity via fMRI or EEG.44 Research has found that as many as 25% of behaviorally non-responsive patients in intensive care units may retain this form of covert awareness.44 This has led to recommendations that advanced neuroimaging be considered before withdrawing life support, except in cases where brain death has been definitively confirmed by catastrophic injury and established guidelines.44
The "Higher Brain" Debate and Future Directions
Some researchers argue for a "higher brain" definition of death, postulating that the irreversible loss of consciousness alone should constitute death.3 Under this framework, a patient with a functioning brainstem who can still breathe but has permanently lost all cortical function (as in a persistent vegetative state) would be considered dead.11 Currently, however, the "whole brain" standard is required by the UDDA, as the capacity for spontaneous breathing (a brainstem function) is seen as essential to biological life.11
Condition | Behavioral Responsiveness | Brainstem Reflexes | Capacity for Consciousness | Legal Status |
Coma | Absent | Preserved/Variable | Potential for recovery | Alive 8 |
Vegetative State (UWS) | Absent | Preserved | Absent/Unknown | Alive 47 |
Covert Consciousness (CMD) | Absent | Preserved | Preserved (detected via fMRI/EEG) | Alive 44 |
Clinical Death | Absent | Absent (during arrest) | Occasional NDE reports | Dead if not resuscitated 13 |
BD/DNC | Absent | Absent | Irreversibly Lost | Dead 1 |
Conclusions and Clinical Implications
The research conducted over the last twenty years has transformed the study of near-death experiences and brain death from speculative philosophy into a rigorous clinical science. The 2023 revised guidelines for BD/DNC represent the pinnacle of medical efforts to ensure 100% accuracy in the determination of death, integrating adult and pediatric standards to eliminate the risks of false-positive declarations.5
Simultaneously, the AWARE studies have provided empirical evidence that consciousness can persist during clinical death and CPR, often associated with a surge of cortical activity and complex subjective narratives.29 These findings suggest that the dying brain does not simply "shut down" but may enter a state of disinhibited lucidity, facilitated by neurochemical surges of DMT, serotonin, and dopamine.30
While the "bright line" between the living and the dead remains a clinical necessity for organ transplantation and medical-legal clarity, the discovery of covert consciousness and the documentation of veridical NDEs suggest that our understanding of the threshold of death is still evolving.6 For clinicians, the most immediate impact of this research is in the realm of communication. Families facing the catastrophic brain injury of a loved one must be supported with clear, compassionate, and supportive terminology that honors both the biological reality of death and the profound human experience of the final transition.50
Works cited
- Brain Death/Death by Neurologic Criteria (BD/DNC) - DynaMedex, accessed March 6, 2026, https://www.dynamedex.com/management/brain-death-death-by-neurologic-criteria-bd-dnc
- Declaring Brain Death: The Neurologic Criteria | Palliative Care Network of Wisconsin, accessed March 6, 2026, https://www.mypcnow.org/fast-fact/declaring-brain-death-the-neurologic-criteria/
- A survey of American neurologists about brain death: understanding the conceptual basis and diagnostic tests for brain death - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC3310851/
- Brain death: A review of the latest guidelines - BINASSS, accessed March 6, 2026, https://www.binasss.sa.cr/ago24/38.pdf
- Advocacy for State Acknowledgment of the 2023 Brain Death/Death by Neurologic Criteria Guidelines as the Accepted Medical Standards, accessed March 6, 2026, https://www.neurology.org/doi/10.1212/WNL.0000000000214100
- Addressing the Problem of Brain Death Misdiagnosis - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12355472/
- Updated Brain Death Guidance: What Care Teams Need to Know - SCCM, accessed March 6, 2026, https://www.sccm.org/communications/sccm-podcast/sccm-podcast-all-episodes/sccm-pod-533-ccm-updated-brain-death-guidance-what-critical-care-teams-need-to-know
- New Guidance Issued on the Determination of Brain Death, accessed March 6, 2026, https://www.bumc.bu.edu/camed/medicine/articles/2025/new-guidance-issued-on-the-determination-of-brain-death/
- Applying the New Brain Death Guidelines: Updates, Challenges and Controversies - AACN, accessed March 6, 2026, https://www.aacn.org/education/ce-activities/nti25257/applying-the-new-brain-death-guidelines-updates-challenges-and-controversies
- Pediatric and Adult Brain Death/Death by Neurologic Criteria Consensus Guideline, accessed March 6, 2026, https://www.neurology.org/doi/10.1212/WNL.0000000000207740
- Brain death: a clinical overview - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC8925092/
- Brain death, the determination of brain death, and member guidance for brain death accommodation requests - Neurology.org, accessed March 6, 2026, https://www.neurology.org/doi/10.1212/WNL.0000000000006750
- Death in 2025: New Definitions, Ethical Questions & Medical Guidelines - St.Emlyn's, accessed March 6, 2026, https://www.stemlynsblog.org/death-by-neurological-criteria/
- The Spectrum of Consciousness on the Borders of Life and Death - MDPI, accessed March 6, 2026, https://www.mdpi.com/2514-183X/9/4/48
- Explanation of near-death experiences: a systematic analysis of ..., accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC10158795/
- Western Scientific Approaches to Near-Death Experiences - MDPI, accessed March 6, 2026, https://www.mdpi.com/2076-0787/4/4/775
- Near death experience: neuroscience perspective - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC4576755/
- Near-Death-Like Experiences without Life-Threatening Conditions or Brain Disorders: A Hypothesis from a Case Report - Frontiers, accessed March 6, 2026, https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2012.00490/full
- The Near-Death Experience Content (NDE-C) scale - University of Virginia School of Medicine, accessed March 6, 2026, https://med.virginia.edu/perceptual-studies/wp-content/uploads/sites/360/2020/11/Nov-2020-NDE-C-CC.pdf
- A Typology of Near-Death Experiences - ResearchGate, accessed March 6, 2026, https://www.researchgate.net/publication/19135541_A_Typology_of_Near-Death_Experiences
- DMT Models the Near-Death Experience - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC6107838/
- Near-Death Experiences: Neuroscience Perspectives on Near-Death Experiences - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC6170042/
- The veridical Near-Death Experience Scale: construction and a first ..., accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12573288/
- Distressing Near-Death Experiences: The Basics - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC6173534/
- A distressing near-death experience with veridical perceptions during coma: psychiatric and clinical reflections from a rare case - PubMed, accessed March 6, 2026, https://pubmed.ncbi.nlm.nih.gov/41665893/
- Consciousness - NYU Langone Health, accessed March 6, 2026, https://med.nyu.edu/research/parnia-lab/consciousness
- Results of world's largest Near Death Experiences study published, accessed March 6, 2026, https://www.southampton.ac.uk/news/2014/10/07-worlds-largest-near-death-experiences-study.page
- (PDF) AWARE-AWAreness during REsuscitation-a prospective study - ResearchGate, accessed March 6, 2026, https://www.researchgate.net/publication/267755643_AWARE-AWAreness_during_REsuscitation-a_prospective_study
- AWAreness during REsuscitation - II: A multi-center study of ..., accessed March 6, 2026, https://pubmed.ncbi.nlm.nih.gov/37423492/
- Comments on the Results of the AWARE II Study - UNT Digital Library, accessed March 6, 2026, https://digital.library.unt.edu/ark:/67531/metadc2350254/
- Neuro-functional modeling of near-death experiences in contexts of altered states of consciousness - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC9891231/
- Neuro-functional modeling of near-death experiences in contexts of altered states of consciousness - Frontiers, accessed March 6, 2026, https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2022.846159/full
- Recent Report of Electroencephalogram of a Dying Human Brain, accessed March 6, 2026, https://med.virginia.edu/perceptual-studies/wp-content/uploads/sites/360/2023/03/JNDE-Recent-Report-of-Electroencephalogram-Greyson-et-al.pdf
- DMT: Mechanisms, Psychological and Physiological Effects, and Its Dual Role as a Drug of Abuse and Potential Health Benefit - NSUWorks, accessed March 6, 2026, https://nsuworks.nova.edu/cgi/viewcontent.cgi?article=1009&context=hpd_corx_stuarticles
- Neurochemical and Neurophysiological Effects of Intravenous Administration of N,N-Dimethyltryptamine in Rats | bioRxiv, accessed March 6, 2026, https://www.biorxiv.org/content/10.1101/2024.04.19.589047v2.full-text
- Near death experiences: a multidisciplinary hypothesis - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC3769617/
- Near-Death Experiences - Division of Perceptual Studies - University of Virginia School of Medicine, accessed March 6, 2026, https://med.virginia.edu/perceptual-studies/our-research/near-death-experiences-ndes/
- Pam Reynolds case - Wikipedia, accessed March 6, 2026, https://en.wikipedia.org/wiki/Pam_Reynolds_case
- The Shadow of Death: Part 1-Near-Death Experiences: An Update on the Research and the Controversy | Christian Research Institute, accessed March 6, 2026, https://www.equip.org/articles/the-shadow-of-death-part-1-near-death-experiences-an-update-on-the-research-and-the-controversy/
- Near death, explained. - Duke Initiative for Science & Society, accessed March 6, 2026, https://scienceandsociety.duke.edu/near-death-explained/
- Could Pam Reynolds Hear? A New Investigation into the Possibility of Hearing During this Famous Near-Death Experience, accessed March 6, 2026, https://digital.library.unt.edu/ark:/67531/metadc461684/
- Brief Report: A Near-Death Experience with Veridical Perception ..., accessed March 6, 2026, https://digital.library.unt.edu/ark:/67531/metadc937997/
- The veridical Near-Death Experience Scale: construction and a first validation with human and artificial raters - Frontiers, accessed March 6, 2026, https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2025.1661390/full
- An ethical framework to assess covert consciousness | Request PDF - ResearchGate, accessed March 6, 2026, https://www.researchgate.net/publication/389467957_An_ethical_framework_to_assess_covert_consciousness
- Covert consciousness - CDC Stacks, accessed March 6, 2026, https://stacks.cdc.gov/view/cdc/150358/cdc_150358_DS1.pdf
- Covert consciousness | Request PDF - ResearchGate, accessed March 6, 2026, https://www.researchgate.net/publication/377369269_Covert_consciousness
- Functional neuroimaging in disorders of consciousness: towards clinical implementation - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC12233511/
- Full article: Response to Commentaries on “Defining Death: towards ..., accessed March 6, 2026, https://www.tandfonline.com/doi/full/10.1080/15265161.2025.2570658
- Disclosing Results of Tests for Covert Consciousness: A Framework for Ethical Translation, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC11147696/
- Communicating About Death by Neurologic Criteria - Palliative Care Network of Wisconsin, accessed March 6, 2026, https://www.mypcnow.org/fast-fact/communicating-about-death-by-neurologic-criteria/?print=print
- Death by Neurological Criteria: Caring for Families amid Tragedy - PMC, accessed March 6, 2026, https://pmc.ncbi.nlm.nih.gov/articles/PMC6880066/
- Brain Death/Death by Neurologic Criteria Guidance on Communication, Objections, Pregnancy, and Public Trust, accessed March 6, 2026, https://www.neurology.org/doi/10.1212/WNL.0000000000214334